Our History
VNS Health has a rich history that goes back 130 years. In that time, a lot has changed — in the world and at VNS Health — but one thing that remains the same is our mission to improve the health of people in need.
We’ve grown from a few nurses in 1893 to a diverse team of nearly 10,000 individuals in 2022. We have expanded our services from just home care and community programs to include hospice care, personal care, behavioral health, and care management — to name a few — and we created a research center and a line of health plans.
We have grown and evolved, and our goal is to build on our legacy as we create the future of care.
Our Timeline
-
1893
The Beginning of VNS Health
VNS Health was founded in 1893 by Lillian Wald, who was not only the first public health nurse but also one of the most influential pioneers in the history of nursing, public health, and social reform.

-
1916 – 1928
A Focus on Public Health
In the early 1900s, Lilian Wald championed public health projects. During this time, VNS Health provided education to families to prevent the flu, treated children with polio, and drove health mobiles to test for diphtheria. They also provided vaccines throughout the city.

-
1944
VNSNY Officially Becomes Its Own Agency
In 1944, the Visiting Nurse Service of New York (VNSNY) was established as an agency separate from the original Henry Street Settlement. This move allowed our organization to focus on home care and to continue growing and serving the people of New York.

-
1960s
The Beginnings of Who We Are Now
In 1962, VNS Health launched its Home Aide program, and in 1965, Medicare and Medicaid were signed into law. These changes allowed for VNS Health to adopt a team approach to care that included home health aides, speech-language pathologists, and social workers in addition to nurses and rehab therapists. Although it may seem commonplace today, these were once major shifts in the medical field!

-
1980s
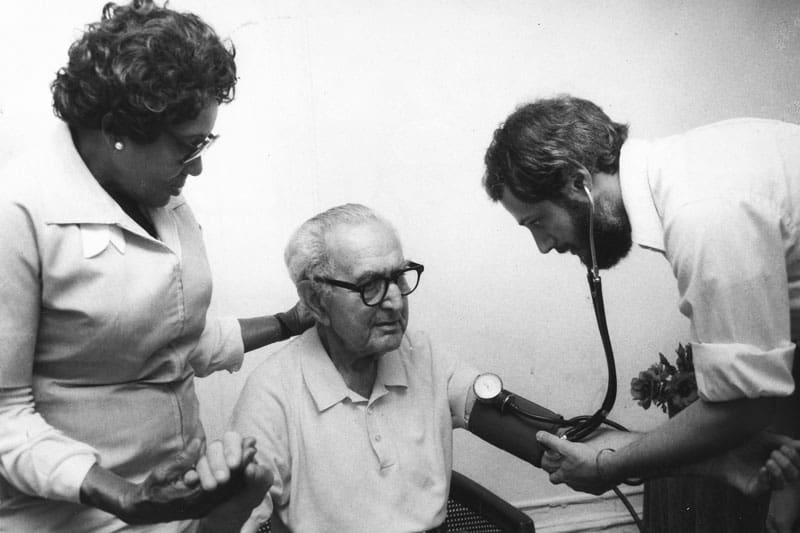
VNS Health and the HIV/AIDS Crisis
VNS Health took action on the front lines of one of the biggest medical crises of the 20th century, caring for people affected by the AIDS epidemic. More than half of those living with AIDS lived in New York City, and VNS Health was the largest home care provider for AIDS patients in the country.
-
1983
New Programs and New Opportunities
The year 1983 was a big one for VNS Health, with the creation of two major programs: Hospice Care and Personal Care. Both programs expanded on our mission of improving the health and well-being of people through high-quality, cost-effective health care in the home and community.

-
1990 – 2010
VNS Health Welcomes the New Millennium
This period saw growth both physically and culturally for VNS Health. The 1990s brought the building of the Center for Home Care Policy & Research as well as our first community center in Lower Manhattan’s Chinatown neighborhood. VNS Health expanded offerings for children and families and in 1998 began offering health plans to help people stay in their homes and communities safely and independently.

-
2010s
Our Commitment to Identity-Affirming Care
VNS Health has long believed that everyone should receive care and support that respects their whole identity. That’s why in the 2010s, we launched key programs specifically for two underserved populations: veterans and members of the LGBTQ+ community. Our identity-specific programs and training for our team members allow us to bring empathetic care to individuals when they need it most.

-
2020
Innovation and Values
The year 2020 demanded that the whole world rethink the way we do things and step up to support one another. VNS Health rose to the challenge, digging into our values and living them out every day. We’ve also established a care management organization and managed services organization, partnering with insurers and hospital networks to provide cost-effective care to high-risk patients and plan members.

-
2022
VNSNY Becomes VNS Health
Throughout our history, we have worked to provide the best possible care and push the needle on home health care. As we look forward to our future and the future of a simpler and more caring health care system, we see clearly how we can play a vital role — and that we need a name change to match. For more than a century, our organization has expanded and evolved. Our new name, VNS Health, builds on our legacy and shows the full spectrum of what we do.
